Fungal ear infection treatment & symptoms
Fungal ear infection treatment & symptoms
3 minutes
Published: 11 January 2022
What is an ear infection?
A fungal ear infection also know as otomycosis typically affects the outer ear - the area from your ear hole to your eardrum (known as the auditory canal).
It can affect one or both ears, and your ear may become red and inflamed. The skin can become itchy and dry, and you might also notice a smelly, discoloured discharge coming from your ear.
But there’s no need to worry. While fungal ear infections are unpleasant, they can be treated quite easily. Here, we’ll discuss some of the key information around fungal ear infection, including how it can be treated.
What are the symptoms?
Fungal ear infections can cause a range of symptoms in one or both ears, including:
• Itching - more common and often worse for infections caused by fungi than by bacteria
• Redness - most likely in the outer part of the ear canal
• Inflammation - your ear may become swollen
• Hearing problems - you may notice a ringing in your ear, or that your ear feels ‘full’
• Pain - your ear could become painful or uncomfortable
• Discharge - look out for a thick fluid coming from your ear. It’s usually yellow, but can be green, black, white or grey
• Flaky skin - the skin around and inside your ear hole can become flaky
You may not experience every one of these symptoms, but if you’re at all concerned or develop dizziness, a high temperature (fever), or are in a lot of pain, you should speak to your doctor.
What are the causes?
Most fungal ear infections are caused by two types of fungus: aspergillus (the most likely cause) and candida.
As fungi prefer a warm, moist environment, there are certain activities that can increase your likelihood of developing a fungal ear infection, including water sports such as swimming or SCUBA diving. You’re also at greater risk during the summer, or if you live in a warm or tropical climate.
You should also reduce how often you use cotton buds, as they can remove protective wax (cerumen) from within your ear canal, providing any fungus with more favourable conditions.
You’re also at greater risk if you have a chronic medical or skin condition, such as:
• Diabetes
• A weakened immune system
• Eczema
• Trauma to your ear canal
What is the diagnosis?
If you have any symptoms of fungal ear infection, it’s important to see your doctor so that they can make a positive diagnosis and provide you with the best treatment.
Make sure you give them any relevant information - including details of any illnesses you have, whether you’ve recently been swimming or SCUBA diving, or whether you’ve just come back from a tropical holiday.
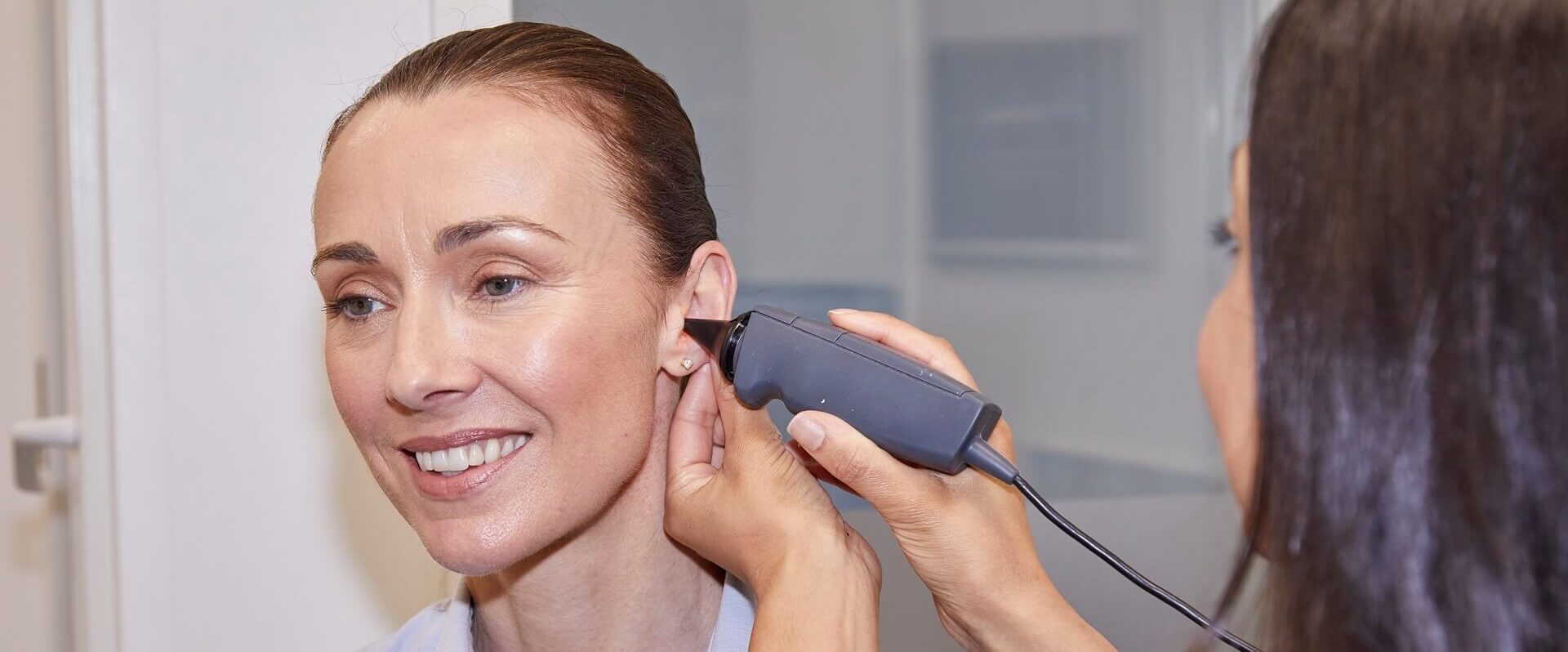
Once they have any necessary details, your doctor will carry out a physical exam of your ears using an otoscope. This will help them get a better look at your ear canal and eardrum.
If you have any discharge, fluid or build-up, your doctor might also take swabs so they can determine whether the problem is caused by fungi or bacteria. This might cause some discomfort, especially if your ear is particularly swollen.
What treatments are available?
Your doctor will let you know which is the best treatment for you, but it is likely to be one of the following:
Cleaning
This is the first step. If your ear is particularly crusted up, or if discharge has built up within your ear, your doctor will use swabs, a syringe or a suction tool to gently and effectively remove it.
While it can be uncomfortable and may need to be done more than once, this process can reduce the chance of the fungus coming back. But it’s important to avoid swimming - and ignore the temptation to scratch your ear - until the infection has completely cleared up.
Ear drops
Your doctor may prescribe antifungal ear drops to help clear the infection. If so, it’s important that you follow their advice and use them as directed until the infection has completely cleared up.
Topical medication
Antifungal creams or ointments can also effectively treat fungal ear infections. These need to be applied to your outer ear, where they will help relieve any hard crusts that have formed as a result of discharge, and treat the underlying infection.
Oral medication
It may be necessary for you to take oral antifungal medication, such as itraconazole or voriconazole, to combat the infection - particularly if other treatments haven’t been successful.
Your doctor will advise which is most suitable for you.
Whichever method of treatment you undergo, it’s important to keep your ear dry and avoid scratching it. And if the infection doesn’t clear up, make sure you revisit your doctor for further treatment or advice.
Frequently asked questions
Author
Boots Hearingcare
Boots Hearingcare



